Keratoconus is a progressive eye condition that affects the shape of the cornea, leading to vision problems over time. The cornea gradually becomes thinner and bulges outward into a cone-like shape, distorting how light enters the eye. This condition often begins in the teenage years or early adulthood and may worsen gradually over several years. Early diagnosis is important to slow progression and protect vision. With modern treatment options, keratoconus can be effectively managed and, in many cases, stabilized.
Key Takeaways
- Keratoconus is a progressive eye condition in which the cornea thins and bulges into a cone shape, causing distorted vision.
- Symptoms include blurry vision, light sensitivity, and frequent changes in eyeglass prescriptions.
- Treatment ranges from glasses and contact lenses to advanced options such as corneal cross-linking or corneal transplantation.
What is Keratoconus?
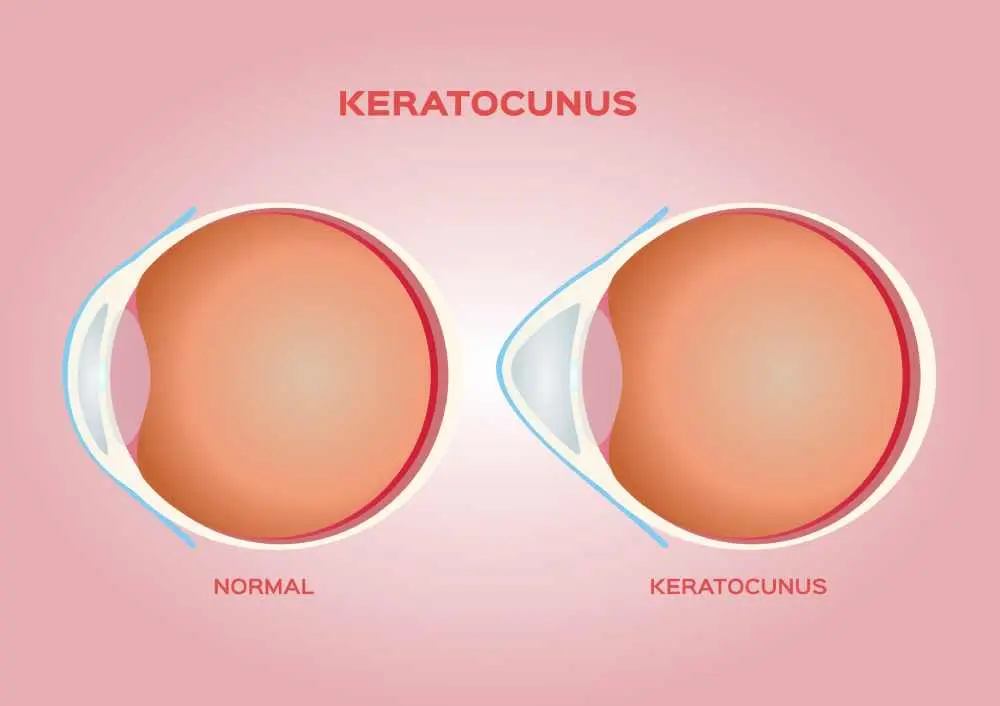
Keratoconus is an eye disorder in which the normally round cornea becomes thin and develops a cone-like shape. This structural change affects the eye’s ability to focus light properly, leading to blurred or distorted vision. The condition usually affects both eyes, although one eye may be more severely affected. Over time, the irregular shape of the cornea can lead to increasing visual impairment. Keratoconus typically develops gradually and may progress over many years.
How does keratoconus affect your vision?
Keratoconus affects vision by altering the shape of the cornea, causing it to thin and bulge outward into a cone-like form. This irregular shape prevents light from focusing properly on the retina, resulting in blurred and distorted vision. Patients may experience glare, halos around lights, and increased sensitivity to light, especially at night. As the condition progresses, vision may become more difficult to correct with standard glasses.
What are Keratoconus Symptoms?
Symptoms of keratoconus often develop gradually and become more noticeable as the condition progresses. Vision changes are usually the first sign, and they may worsen over time. Early symptoms can sometimes be corrected with glasses, but later stages may require more advanced treatment. Recognizing symptoms early helps prevent further vision deterioration.
Common symptoms include:
- Blurred or distorted vision
- Increased sensitivity to light (photophobia)
- Glare and difficulty with night vision
- Frequent changes in eyeglass prescription
- Double vision in one eye
- Seeing halos around lights
What Causes Keratoconus?
The exact cause of keratoconus is not fully understood, but it is believed to involve a combination of genetic and environmental factors. In some cases, the condition runs in families, suggesting a hereditary component. Repeated eye rubbing and certain underlying conditions may also contribute to its development. The weakening of the cornea structure plays a key role in its progression. Understanding possible causes helps guide early intervention and management.
Common causes and contributing factors include:
- Genetic predisposition
- Frequent or vigorous eye rubbing
- Weakening of corneal structure
- Associated medical conditions
- Environmental factors
What are the Risk Factors for Keratoconus?
Certain factors can increase the likelihood of developing keratoconus. These risks are often related to genetics, behavior, or underlying health conditions. People with a family history of keratoconus are at higher risk. Identifying risk factors allows for earlier monitoring and diagnosis.
Risk factors include:
- Family history of keratoconus
- Chronic eye rubbing
- Allergic conditions
- Genetic disorders
- Young age
What are the Complications of This Condition?
Keratoconus can lead to serious complications if it progresses without treatment. These complications mainly affect vision and corneal health. In advanced cases, permanent damage may occur. Early management is important to prevent these outcomes.
Possible complications include:
- Corneal scarring
- Sudden swelling of the cornea
- Severe vision loss
- Difficulty wearing contact lenses
- Need for corneal transplant
How is Keratoconus Diagnosed?
Keratoconus is diagnosed through a comprehensive eye examination and specialized imaging tests. Eye care specialists evaluate the shape and thickness of the cornea to detect abnormalities. Early diagnosis is crucial, as the condition can progress over time. Advanced imaging techniques can identify keratoconus even in its early stages.
Diagnostic methods include:
- Vision tests
- Slit-lamp eye examination
- Corneal topography
- Keratometry
- Detailed medical and family history
What’s the Treatment for Keratoconus?
Treatment for keratoconus depends on the severity and progression of the condition. The main goals are to improve vision and slow or stop the progression. Early stages can often be managed with corrective lenses, while advanced cases may require surgical intervention. Modern treatments have significantly improved outcomes.
Treatment options include:
- Eyeglasses or soft contact lenses
- Rigid or scleral contact lenses
- Corneal collagen cross-linking
- Intrastromal corneal ring implants
- Corneal transplant
Can Keratoconus Be Prevented?
Keratoconus cannot always be prevented, especially when genetic factors are involved. However, certain habits may reduce the risk of progression. Protecting eye health and avoiding harmful behaviors are key strategies. Early monitoring also plays an important role in prevention.
Prevention tips include:
- Avoid rubbing the eyes
- Manage allergies effectively
- Have regular eye examinations
- Follow medical advice if diagnosed early
- Use prescribed corrective lenses properly
Which department should I visit?
Patients with symptoms of keratoconus should consult the Ophthalmology (Eye Diseases) department. Eye specialists can provide accurate diagnosis and recommend appropriate treatment options.

 Let Us Call You
Let Us Call You




































